When traditional wound care isn’t delivering the results patients need, medical professionals often turn to advanced therapies that can accelerate the healing process. Hyperbaric oxygen therapy has emerged as a powerful tool in treating stubborn wounds that refuse to heal through conventional methods. This treatment involves breathing pure oxygen in a pressurized chamber, creating conditions that dramatically enhance the body’s natural healing capabilities.
Understanding how this therapy works can help patients and caregivers make informed decisions about wound care options. Let’s explore the five key mechanisms through which this innovative treatment accelerates wound recovery.
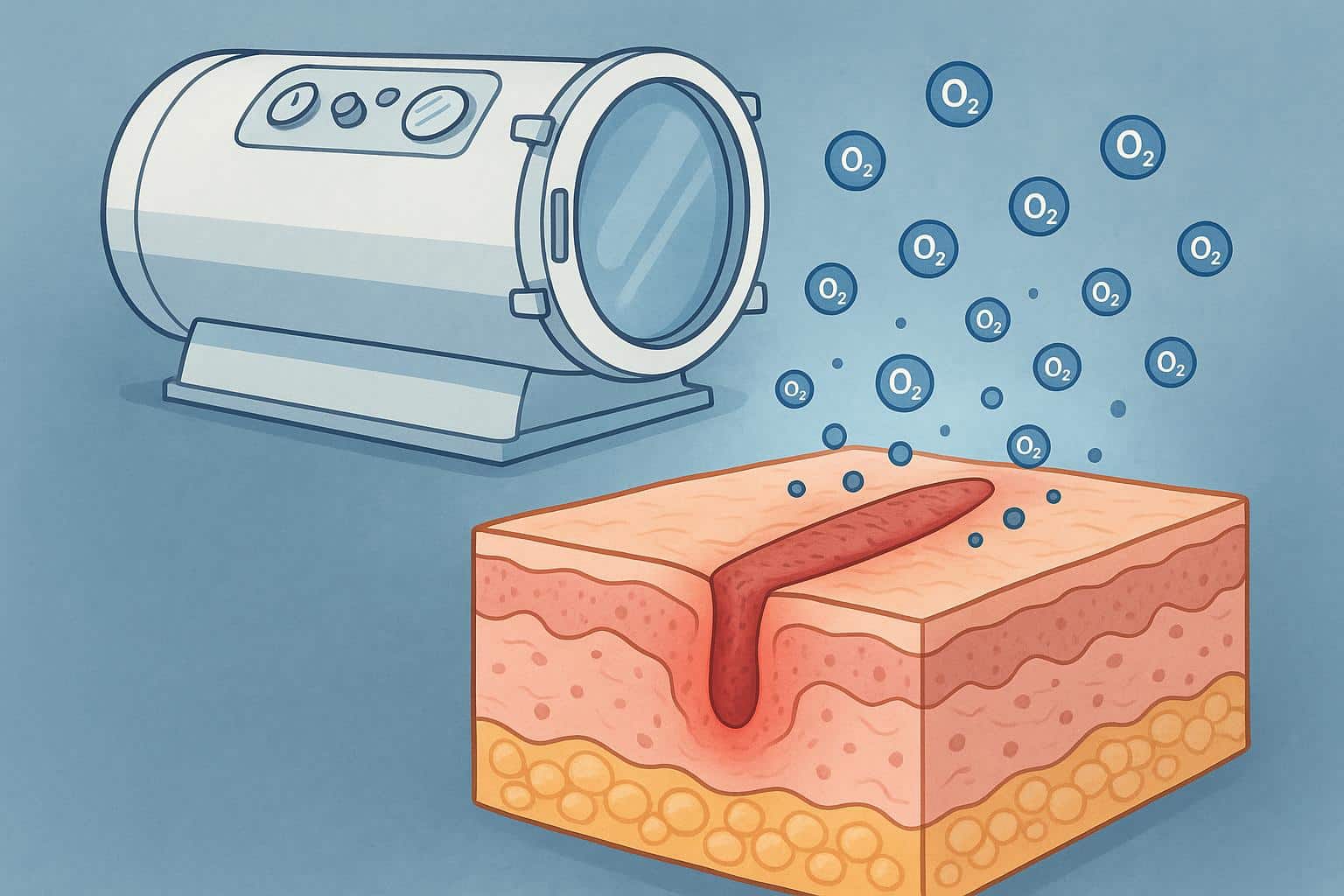
Flooding Damaged Tissue with Oxygen
The human body needs oxygen to heal, but damaged tissue often struggles to receive adequate amounts through normal circulation. During hyperbaric wound treatment, patients breathe 100% oxygen while inside a pressurized chamber, which increases the amount of oxygen dissolved in the blood plasma by up to 20 times normal levels.
This oxygen-rich blood reaches even the most compromised areas of wounded tissue. Cells that were starving for oxygen suddenly receive the fuel they need to repair themselves and regenerate. This process is particularly crucial for wounds with poor blood flow, such as diabetic ulcers or radiation-damaged tissue.
The elevated oxygen levels persist in the tissues even after treatment ends, providing extended healing benefits. This sustained oxygen availability gives cells the resources they need to continue repair work between therapy sessions.
Stimulating New Blood Vessel Growth
One of the most remarkable effects of hyperbaric therapy is its ability to trigger angiogenesis, the formation of new blood vessels. Wounds heal poorly when they lack adequate blood supply, creating a vicious cycle where damaged tissue cannot receive the nutrients and oxygen needed for recovery.
The high-pressure oxygen environment signals the body to grow new capillaries into the wound area. These fresh blood vessels establish permanent pathways for oxygen and nutrients to reach healing tissue. Over time, this improved vascular network transforms the wound bed from a hostile environment into one conducive to healing.
This process doesn’t happen overnight, but with repeated treatments, patients often see dramatic improvements in wound appearance and reduction in size. The new blood vessels continue to support healing long after therapy concludes.
Enhancing White Blood Cell Function
The immune system plays a critical role in wound healing, and white blood cells serve as the body’s primary defense against infection. However, these infection-fighting cells require substantial amounts of oxygen to function effectively, especially when battling bacteria in wounded tissue.
Hyperbaric therapy supercharges white blood cells, enabling them to kill bacteria more efficiently. The elevated oxygen levels also help these cells produce reactive oxygen species that destroy harmful microorganisms. This enhanced immune function is particularly important for chronic wounds that have become infected or colonized with bacteria.
Additionally, the oxygen-rich environment itself creates conditions that many bacteria find inhospitable. Anaerobic bacteria, which thrive in low-oxygen environments, struggle to survive when oxygen levels spike during treatment sessions.
Reducing Inflammation and Swelling
Chronic inflammation often prevents wounds from progressing through normal healing stages. Swelling restricts blood flow, creates pressure on surrounding tissue, and can cause additional damage to already compromised areas.
Hyperbaric oxygen therapy helps regulate the inflammatory response, reducing excessive swelling while still allowing the beneficial aspects of inflammation to proceed. The treatment constricts blood vessels slightly, which decreases fluid leakage into tissues without compromising oxygen delivery thanks to the dramatically increased oxygen concentration in the blood.
This reduction in swelling creates space for new tissue growth and improves the overall wound environment. Patients often report decreased pain and improved mobility in affected areas as inflammation subsides.
Activating Growth Factors and Stem Cells
The body’s healing mechanisms rely on chemical signals called growth factors that tell cells when and how to repair damage. Hyperbaric therapy stimulates the release of these crucial signaling molecules, jumpstarting healing processes that may have stalled.
The treatment also mobilizes stem cells from bone marrow, sending them into circulation where they can travel to wounded areas. These versatile cells can transform into various tissue types needed for repair, from skin cells to blood vessel cells.
This activation of the body’s regenerative potential represents one of the most exciting aspects of hyperbaric therapy. Rather than simply treating symptoms, it harnesses the body’s own healing intelligence to address the root causes of delayed wound healing.
Moving Forward with Confidence
Hyperbaric oxygen therapy offers hope for patients struggling with wounds that resist conventional treatment. By addressing multiple aspects of the healing process simultaneously, this approach can transform outcomes for diabetic ulcers, radiation injuries, surgical wounds, and other challenging conditions. If you’re dealing with a wound that won’t heal, discussing hyperbaric therapy with your healthcare provider could open doors to faster, more complete recovery.

